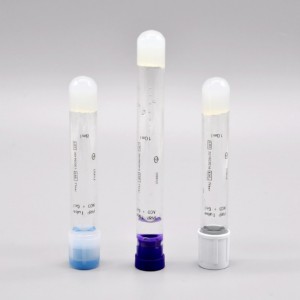
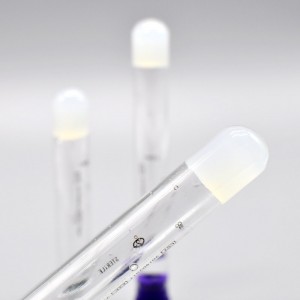
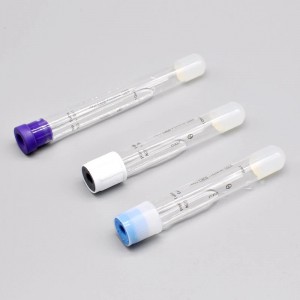
Blood Collection PRP Tube
Short Description:
Platelet Gel is a substance that is created by harvesting your body’s own natural healing factors from your blood and combining it with thrombin and calcium to form a coagulum. This coagulum or “platelet gel” has an extremely wide range of clinical healing uses from dental surgery to orthopedics and plastic surgery.
Platelet-rich plasma (PRP) is also known as platelet-rich growth factors (GFs), platelet-rich fibrin (PRF) matrix, PRF, and platelet concentrate.
The concept and description of PRP started in the field of hematology. Hematologists created the term PRP in the 1970s in order to describe the plasma with a platelet count above that of peripheral blood, which was initially used as a transfusion product to treat patients with thrombocytopenia.
Ten years later, PRP started to be used in maxillofacial surgery as PRF. Fibrin had the potential for adherence and homeostatic properties, and PRP with its anti-inflammatory characteristics stimulated cell proliferation.
Subsequently, PRP has been used predominantly in the musculoskeletal field in sports injuries. With its use in professional sportspersons, it has attracted widespread attention in the media and has been extensively used in this field. Other medical fields that also use PRP are cardiac surgery, pediatric surgery, gynecology, urology, plastic surgery, and ophthalmology.
More recently, the interest in the application of PRP in dermatology; i.e., in tissue regeneration, wound healing, scar revision, skin rejuvenating effects, and alopecia, has increased.
Wounds have a proinflammatory biochemical environment that impairs healing in chronic ulcers. In addition, it is characterized by a high protease activity, which decreases the effective GF concentration. PRP is used as an interesting alternative treatment for recalcitrant wounds because it is a source of GFs and consequently has mitogen, antigenic, and chemotactic properties.
In cosmetic dermatology, a study performed in vitro demonstrated that PRP can stimulate human dermal fibroblast proliferation and increase type I collagen synthesis. Additionally, based on histological evidence, PRP injected in human deep dermis and immediate sub dermis induces soft-tissue augmentation, activation of fibroblasts, and new collagen deposition, as well as new blood vessels and adipose tissue formation.
Another application of PRP is the improvement of burn scars, postsurgical scars, and acne scars. According to the few articles available, PRP alone or in combination with other techniques seems to improve the quality of the skin and leads to an increase in collagen and elastic fibers.
In 2006, PRP has started to be considered a potential therapeutic tool for promoting hair growth and has been postulated as a new therapy for alopecia, in both androgenetic alopecia and alopecia aerate. Several studies have been published that refer to the positive effect PRP has on androgenetic alopecia, although a recent meta-analysis suggested the lack of randomized controlled trials. As stated by the authors, controlled clinical trials are considered the best way to provide scientific evidence for a treatment and avoid potential bias when assessing efficacy.